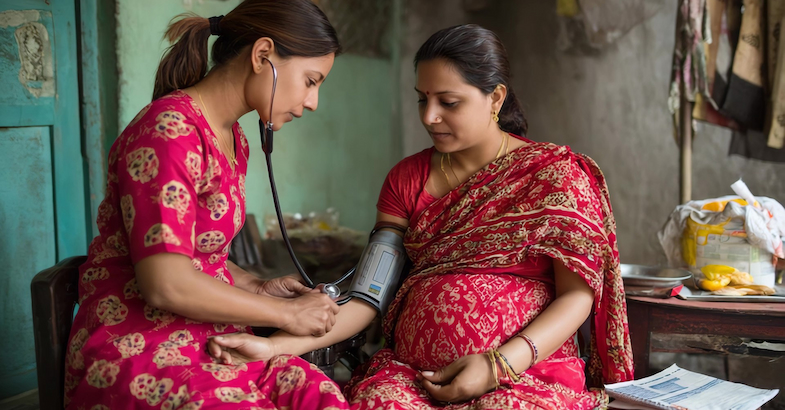
In Punjab, around 40 percent of adults have hypertension, yet fewer than half are aware of it and only a fraction has it under control. Similarly, about 14 percent live with diabetes, with persistent gaps in awareness and management. In several cases, these conditions remain undetected, often due to irregular routine screening, especially in rural areas. As a result, people often learn about them only when symptoms worsen or during unrelated health visits. These figures point to a quiet crisis: conditions that are largely preventable and manageable, yet remain uncontrolled for many.1
During my field interactions with locals, I identified a striking pattern. Many households pay for private care even when government services are available for free or at subsidized rates. Government facilities in rural Punjab, much like in other parts of India, comprise primary health centers and sub-ceinters designed as frontline facilities, providing consultations, basic diagnostics, and medicines at little or no cost. Ideally, this should mean that affordable or ‘free’ healthcare is accessible to rural areas. From afar, it does seem so, however, the ground reality is different.
Almost every household my team and I spoke to had spent on healthcare in recent months, either for consultations, diagnostic tests, medicines, or transport. This trend raised a simple but important question for me: why were people continuing to pay for healthcare services that, in principle, were available for free?
Over several conversations with villagers, a clearer picture began to emerge. I began to see that the cost of healthcare is not just limited to the boundaries of a clinic or hospital. The distance to the health facility, lack of proper transport, and long queues and waiting times at government facilities often mean losing a full day of paid work, almost every month, particularly for those living with chronic ailments. Several families cannot afford that loss, in addition to the financial strain they already bear due to the disease. In this sense, ‘free’ healthcare still carries hidden costs, of time, travel, lost wages, and uncertainty.
As a result, while services may technically be available, timely and convenient access to them often remains uneven. In many conversations, even basic screenings came up as something that required travelling to distant facilities. For many villagers, at least for regular screenings and non-invasive diagnostics, a nearby private provider who charges a modest fee but offers quick and predictable service often feels like a more practical option. These conversations revealed a nuanced gap: the healthcare facilities were not absent, but easy and equitable access to care within the village was missing.
In this context, the presence of a trained community-based health worker can bring basic services closer to households, helping in early detection and continuous monitoring, while reducing financial and logistical costs. In my project at ISB’s Max Institute of Healthcare Management, we are studying the impact of this model in rural Punjab, where local women are being empowered as Community Health Entrepreneurs to deliver last-mile healthcare in their communities.2 These women serve as locally embedded providers who can offer basic screening, counselling, and non-invasive diagnostics at the doorstep, making it easier for households to access routine care and detect health risks earlier without needing to travel repeatedly to distant and overcrowded facilities.
Not only in Ropar’s villages but in rural areas across India, the ongoing demographic and epidemiological shifts underscore a pressing need to rethink how healthcare is accessed and delivered. Everyday constraints around distance, transport, timing, and service reliability suggest that the promise of ‘free’ public healthcare does not always translate into easy access for many families. What people seemed to value, across conversations, was not simply the price of care, but its proximity and predictability. Approaches that bring basic health services closer to households may help bridge the gap between what is available on paper and what people are practically able to use. Strengthening last-mile access through community-based providers may, therefore, be an important step toward translating affordability into actual accessibility.
1International Institute for Population Sciences (IIPS) and ICF. 2021. National Family Health Survey (NFHS-5), India, 2019-21: Punjab. Mumbai: IIPS
2The Sehat Sevika programme is an initiative of Bahaar Foundation, in partnership with the Punjab Development Commission, that trains local women as Community Health Entrepreneurs to deliver basic health services at the village level in Rupnagar district, Punjab. See bahaarfoundation.org.
*The views expressed in this article are solely the personal opinions and reflections of the author(s) and do not necessarily reflect the objectives of the study they are part of.
Author’s Bio:

Vedushi M Jain
Public health researcher
Vedushi M Jain is a public health researcher with a clinical background in dentistry and expertise in healthcare research, administration, and policy. She is currently a Research Analyst at the Max Institute of Healthcare Management, Indian School of Business, where she works on strengthening primary healthcare delivery through evidence-based research and programme evaluation.
Her work spans health systems research, drawing on mixed-methods approaches, with a particular focus on projects aimed at advancing health equity.